-
Home
-
Pressure Injury Prevention: Guidelines and Best Practices
Pressure Injury Prevention: Guidelines and Best Practices
January 2, 2024
 Pressure injuries, such as pressure sores or ulcers, are a common and serious problem faced by patients who are unable to reposition themselves or those with limited mobility. These injuries occur when prolonged pressure on soft tissue causes tissue damage and limits blood supply to the area, leading to a greater risk of infection and further complications. This article will provide some guidelines and best practices for reducing the risk of pressure injuries.
Pressure injuries, such as pressure sores or ulcers, are a common and serious problem faced by patients who are unable to reposition themselves or those with limited mobility. These injuries occur when prolonged pressure on soft tissue causes tissue damage and limits blood supply to the area, leading to a greater risk of infection and further complications. This article will provide some guidelines and best practices for reducing the risk of pressure injuries.
Clinical Practice Guidelines
Clinical practice guidelines for the prevention and treatment of pressure ulcers, developed by the National Pressure Ulcer Advisory Panel, provide evidence-based recommendations for preventing and treating pressure injuries. These guidelines include recommendations on assessment, repositioning, nutrition and hydration, use of support surfaces, incontinence management, monitoring and documentation, patient and caregiver education, and regular training.
Risk Assessment
The first step in preventing pressure injuries is identifying patients who are at high risk, such as those with spinal cord injuries or those with existing pressure injuries. Regular skin assessments play a pivotal role in identifying changes or potential issues, with a particular focus on bony prominences and areas with limited fat padding. Utilizing validated pressure injury risk assessment tools helps identify risk factors such as immobility, incontinence, malnutrition, and age.
Repositioning
Repositioning is fundamental in preventing pressure injuries and is particularly crucial for patients who are bedridden or have limited mobility. A structured and routine schedule for turning and repositioning patients at intervals of every two hours is essential. This regular repositioning helps alleviate sustained pressure on vulnerable areas, such as bony prominences, thereby promoting adequate blood flow and preventing the development of pressure injuries.
Nutrition and Hydration
Ensuring that patients receive adequate nutrition is crucial, as malnutrition can contribute to skin vulnerability. Collaboration with dietitians to develop appropriate nutritional plans is recommended, along with maintaining proper hydration levels to promote skin elasticity and overall skin health.
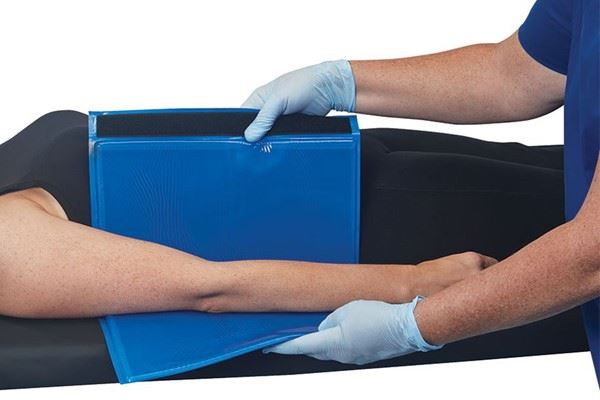
Support Surfaces
Selecting appropriate support surfaces based on individual patient needs is critical. Mattresses, patient positioners, and other specialized surfaces can aid in preventing injuries through pressure redistribution and protection against shear. These surfaces are used in both hospital environments—such as the operating room—and long-term care facilities. Proper support surfaces play a vital role in alleviating pressure on vulnerable regions, such as bony prominences, ensuring a more comfortable and supportive environment for patients.
Incontinence Management
Prolonged exposure of the skin to moisture and irritants due to incontinence significantly increases the vulnerability of the skin, making it more prone to breakdown. Proper incontinence management is crucial in mitigating these risks, and one key preventive measure involves the use of moisture-barrier creams or ointments. These products create a protective barrier on the skin's surface, acting as a shield against the detrimental effects of prolonged moisture and potential irritants.
Monitoring and Documentation
Establishing a robust system for the continuous monitoring and documentation of skin integrity is critical in preventing pressure injuries. This includes pressure injury risk assessments, preventive measures, and timely responses to any skin breakdown or signs of pressure injuries. By fostering a culture of meticulous monitoring and documentation, healthcare providers enhance their ability to identify, address, and prevent pressure injuries.
Education and Regular Training
Education for patients, caregivers, and healthcare staff is paramount in pressure injury prevention, involving. Providing guidance on repositioning techniques, skincare, and the use of assistive devices ensures a comprehensive approach. Continuous training for healthcare staff on pressure injury prevention protocols and best practices is essential. Furthermore, establishing a system for continuous quality improvement involves the constant evaluation of prevention measures and allows for adjustments as needed.
Treatment
The treatment of existing pressure injuries, such as pressure ulcers, involves wound care and reducing the pressure on affected areas. It is important to debride dead tissue and promote healing, either through surgical intervention or the use of dressings. If the patient's mobility is limited, it may be necessary to use a bed that alternates pressure points or a special mattress to reduce pressure.
Palliative Care
Pressure injuries are a common problem in palliative care patients, who are at an increased risk of pressure injuries. Preventing pressure sores is particularly important as these patients often spend long periods of time in bed. Best practices include regular skin assessment, appropriate positioning, and the use of pressure-relieving devices.
Pressure Injury Prevention Toolkit
The Pressure Injury Prevention Toolkit, developed by the Agency for Healthcare Research and Quality, provides clinicians with evidence-based interventions for preventing pressure injuries. This toolkit includes strategies for assessing risk factors, repositioning techniques, and tools for educating patients and their families about pressure injury prevention.
Preventing pressure injuries should be a priority in all healthcare settings. Best practices for prevention include identifying patients at high risk, repositioning patients every two hours, using pressure-relieving devices, and keeping the skin clean and dry. By following evidence-based guidelines and best practices, healthcare professionals can significantly reduce the incidence of pressure injuries and improve patient outcomes.