-
Home
-
How to prevent bed sores
How to prevent bed sores
April 20, 2015
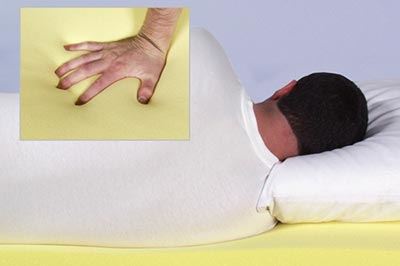
Long-term care providers need to monitor a range of health status factors in their residents. Depending on these individuals' medical conditions, such factors may include vigilance over blood sugar, blood pressure or the tendency to wander around. For those who have mobility issues that keep them bound to a chair or bed, caregivers need to be aware of bed sores from long-term care.
As with any medical issue, prevention and early treatment are the most important approaches to protecting residents' health. James Spahn, M.D., FACS, founder of medical supply company EHOB, wrote a guest column in Long Term Care News, in which he discussed how residents' resting surfaces can play a pivotal role in the development of bed sores.
"When analyzing the relationship between soft-tissue injury and support surfaces for [bed sore] treatment and prevention, caregivers must realize support surfaces deliver unwanted gradient pressure and/or shear mechanical stresses, resulting in soft tissue distortion," Spahn wrote. "This distortion causes endothelial damage and can result in ischemia and possible infarction of the soft tissue at risk. The scientific disciplines of chemistry, physics, and mechanics can help caregivers understand mechanical stresses delivered to the resident at risk for [bed sore] development."
Make sure clinicians are educated
According to Spahn, clinicians are more inclined to be vigilant about the prevention and treatment of bed sores if they are educated on the severity of these problems. Once they are aware of the dangers, they will know that complete resident assessments are one of the first steps to take. This means assessing individuals for risk factors of bed sores, which include impaired mental status, incontinence, immobility, nutritional deficiencies, inactivity, exposure to moisture and others, according to the National Pressure Ulcer Advisory Panel. This may reveal issues that can be addressed immediately, such as fluid intake. From there, assessments must be conducted regularly at least once a week, based on the residents' needs.
Whether prevention or treatment is what is needed, a resting surface that equalizes load redistribution can be valuable, to the point of reducing the number of bed sores by as much as 90 percent, according to Spahn. When these devices are used, special attention is needed for the bony prominences. Additionally, the NPUAP recommended that bed-bound residents be repositioned every two hours, while chair-bound people who are able to move should shift their weight every 15 minutes.